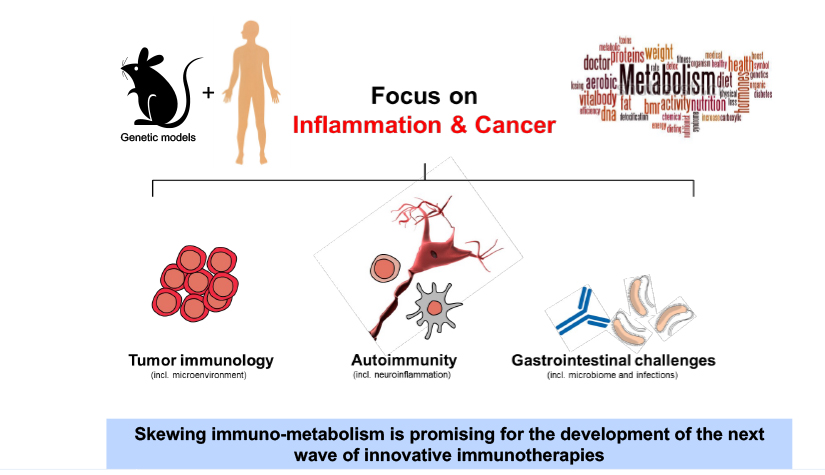
A glimpse into our research
The immune system is crucial for a healthy body to function and protects us from severe infection. However, a dysregulated immunity can cause inflammation, autoimmune diseases and cancer. The control of immune cell metabolism has emerged as a powerful way to regulate immunity and is at the core of our research activities.